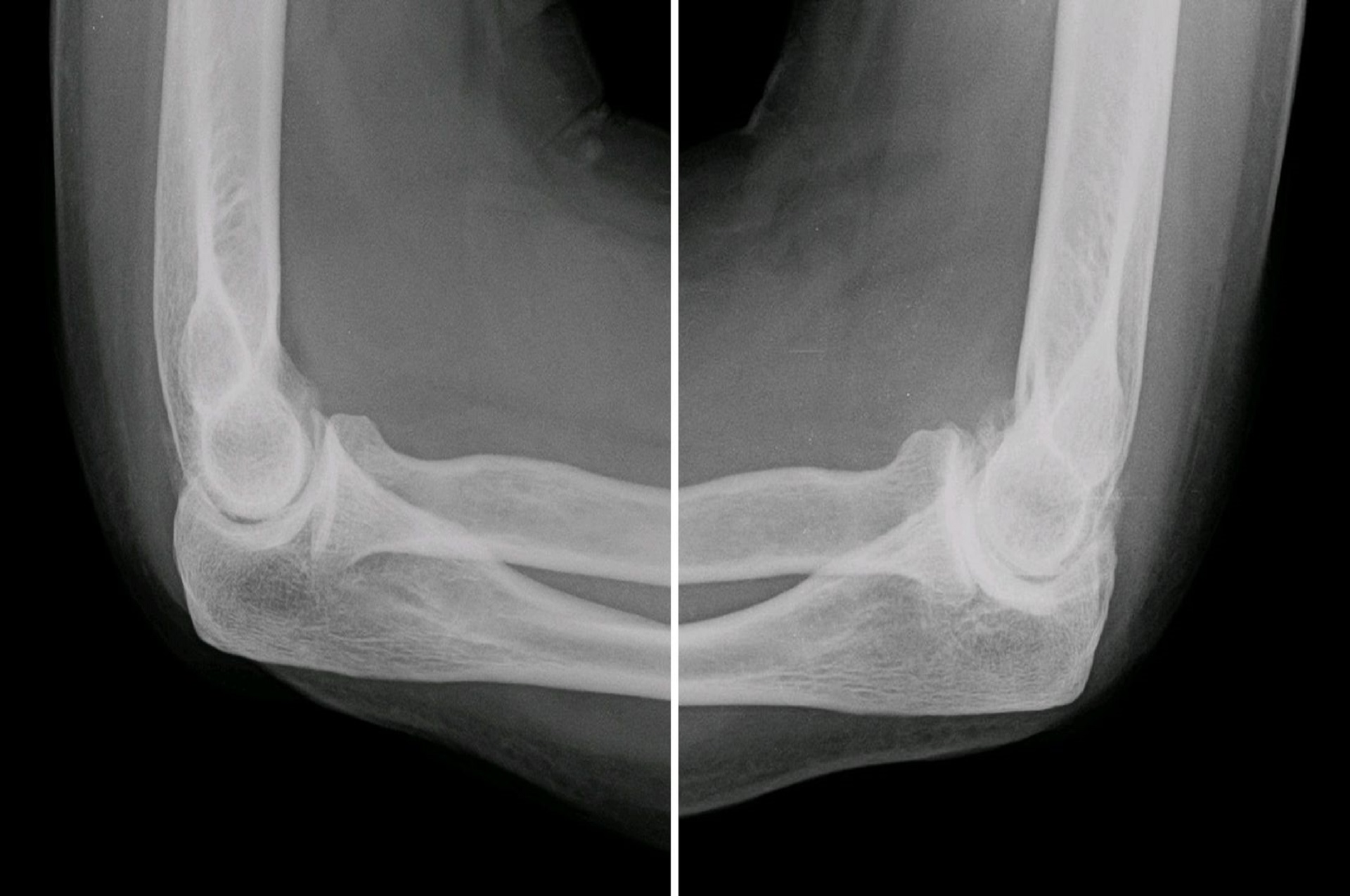
Osteoarthritis: The Progressive Joint Disease Affecting Millions of Americans
The National Arthritis Foundation describes osteoarthritis (OA) as the most common chronic condition of the joints, affecting approximately 27 million Americans. OA can affect any joint, but it occurs most often in knees, hips, lower back and neck, small joints of the fingers and the bases of the thumb and big toe.
With the process of aging comes the wearing of cartilage on the bone, resulting in the loss of a natural cushion between bones and joints. In the case of Osteoarthritis or OA, the cartilage wears down, causing friction that causes pain. If left untreated for an extended time the pain can increase and may cause a brittle residual bone that is extremely susceptible to breaking especially with an accidental fall. This can be a traumatic experience especially for an elderly person experiencing much of this for the first time. The Arthritis Foundation explains “As OA worsens over time, bones may break down and develop growths called spurs. Bits of bone or cartilage may chip off and float around in the joint. In the body, an inflammatory process occurs and cytokines (proteins) and enzymes develop that further damage the cartilage. In the final stages of OA, the cartilage wears away and bone rubs against bone leading to joint damage and more pain.”
So what are health care providers and physicians doing about Osteoarthritis? There is not a single fix for OA, but there are comprehensive multidisciplinary approaches that combine an overarching treatment algorithm to help a patient with this condition. Aside from opioids, narcotics and surgical procedures, which can be undesirable by the patient in many instances; one of the most popular minimally invasive procedures garnishing a lot of attention is needle guided injections utilizing hyaluronic acid or hyalgan. This can be used in many cases as a topical agent to treat burns, bed sores and wounds, but when injected can help relieve knee pain by reintroducing a similar cartilage-like cushion which in effect lubricates the joints and bones that are rubbing against each other.
Medical providers that use fluoroscopy units such as C-Arms or digital ultrasounds are far more likely to have their patients recover quickly than doctors executing the injection based on judgement alone. With resonance-based imaging, it takes the guess work out of the equation and a nurse practitioner or MD may apply the injection with pin point accuracy. After the hyalgan injection, some practices incorporate DME, or durable medical equipment as part of the treatment regimen. An OA knee brace gives added support and comfort to the treated areas allowing for an accelerated recovery curve to take place.
Once the patient has had the brace in place for a set duration of time dependent upon the severity of the condition and doctors recommendation, it is often recommended for the patient to do physical therapy to allow for better readjustment to activities of daily living. Another route being pursued by many doctors who are more progressive is PRP and stem cell therapy. But it is important to note these are still considered experimental in nature and while there is evidence to show that clinical efficacy from these procedures can be quite substantial for conditions like OA. Hyalgen however is backed by the FDA and is still considered the gold standard of treatment for OA in patients, although PRP and Stem Cell are the buzz words of the day and are stirring quite a bit of attention amongst the medical community.
Regardless of the patients preference it is always best to allow the treating physician to make a proper and thorough diagnosis of each patient and allow him/her to assess which treatment regimen would be best suited for the individual. Collectively speaking these treatment parameters come together to help OA patients get out of pain, stay out of pain for long durations of time and drastically improve their overall quality of life.